.jpg)
RCM, EHR/PMS, automation and compliance support
AmeryMED brings billing, coding, credentialing, rule engines, reporting, scheduling and secure cloud workflows into one practical operating model for practices.
What AmeryMED unifies
From eligibility through payment, AmeryMED focuses on the handoffs where revenue, compliance and patient communication usually slow down.

Custom rule engines reduce avoidable errors, enforce payer requirements and standardize repeatable practice workflows.

Claim submission, denial tracking, payment follow-up and reporting designed to improve revenue control.

Cloud-based practice tools for charting, scheduling, patient records, reporting and day-to-day staff coordination.
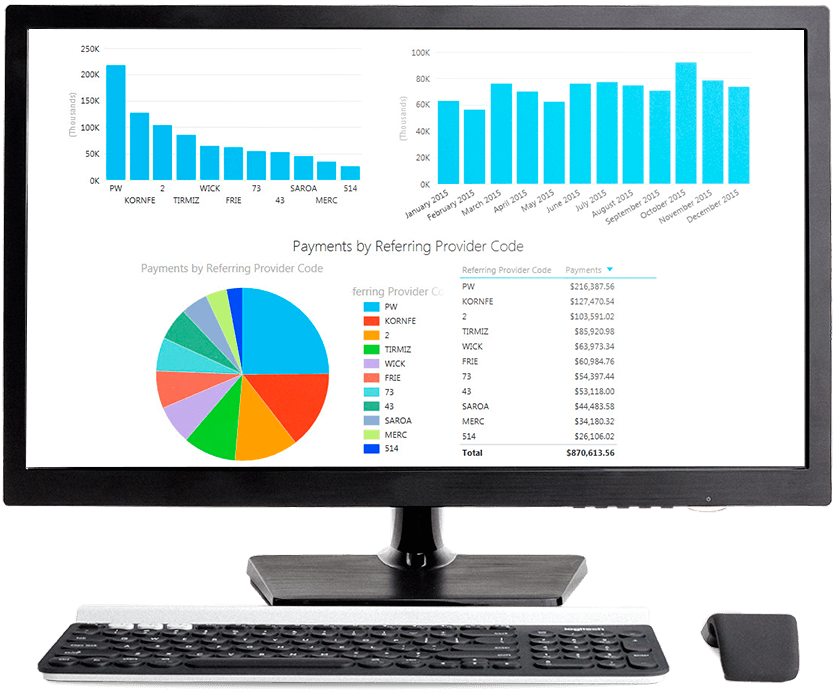
Revenue cycle management
AmeryMED supports practices across the revenue cycle with billing operations, coding accuracy, denial follow-up, eligibility checks, prior authorization and financial reporting.
AmeryMED Web portal
AmeryMED Web gives practices a clearer way to coordinate billing activity, claim follow-up, reports, client communication and administrative oversight from one secure portal experience.
Practice technology
Compliance and quality control
Compliance audit, transcription, practice consulting and credentialing services give teams a stronger operational foundation around e-PHI, documentation and payer participation.

Ready for the next step?
Tell us about your current billing, EHR, automation or compliance needs and we will map the right service path.